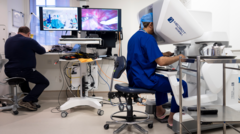
The room in London is silent, save for the low, rhythmic hum of cooling fans. Inside this sterile cocoon, a patient lies anesthetized, their life suspended in that strange, chemical limbo between wakefulness and the void. There is a surgeon here, of course, but they aren't holding a scalpel. They are watching a screen with the intensity of a hawk.
Across the English Channel, over the jagged peaks of the Alps, and deep into the sun-drenched landscape of Bordeaux, France, another man sits at a console. Dr. Alberto Breda is peering into a three-dimensional viewfinder. His fingers are tucked into delicate loops, moving with the grace of a concert pianist. Every flick of his wrist, every micro-adjustment of his thumb, is being translated into light.
That light travels. It dives into fiber-optic cables, pulses through sub-sea tunnels, and screams across international borders at nearly the speed of causality. In London, the robotic arms hovering over the patient mimic those movements with terrifying precision.
This isn't a laboratory simulation. It is the first time in the history of British medicine that a surgeon has removed a cancerous tumor from a patient while standing in a different country.
The Ghost in the Machine
To understand why this matters, you have to understand the traditional tyranny of geography. For decades, if you had a rare, aggressive form of cancer, your survival depended entirely on who lived within a fifty-mile radius of your bed. If the world’s best specialist was in Bordeaux and you were in a London infirmary, you were out of luck. You either traveled while sick—a brutal undertaking—or you settled for the best available local option.
The "Distance Barrier" has always been the silent killer in modern healthcare.
When the robotic arms began to move in that London operating theater, that barrier didn't just crack; it evaporated. We are talking about a radical shift in how we define "presence." In this operation—a complex procedure to remove a kidney tumor—the surgeon’s expertise was decoupled from his physical body.
Consider the technical nightmare of "latency." In the world of online gaming, a delay of a few milliseconds means you lose a match. In the world of remote surgery, a delay of a few milliseconds could mean a punctured artery or a missed margin. The signal had to travel 1,500 miles, be processed by the robot, and reflected back to the surgeon’s eyes fast enough that he felt as though he were touching the tissue himself.
The delay was measured at a staggering 57 milliseconds. To put that in perspective, it takes about 300 to 400 milliseconds for a human to blink. The connection was, for all practical intents, instantaneous.
A Symphony of Glass and Light
The procedure was a partial nephrectomy. It is a high-stakes game of inches. The goal is to excise the malignancy while preserving as much healthy kidney function as possible. One wrong move and the patient faces a lifetime of dialysis.
Dr. Breda, President of the European Association of Urology, wasn't just fighting cancer; he was proving a point. He was navigating the Da Vinci Xi surgical robot via a specialized console provided by the company Saros. As he navigated the internal anatomy of the patient, he was seeing a high-definition, magnified 3D view of the surgical site.
Every time he "felt" the resistance of the tissue, it was through haptic feedback loops that tricked his brain into believing the 1,500 miles of earth and sea between him and the patient didn't exist.
The surgeon in London, acting as the "bedside" assistant, remained ready to intervene, but they never had to. The ghost in the machine was sufficient. The tumor was removed. The bleeding was controlled. The patient woke up hours later, likely unaware that their savior had been enjoying a French espresso shortly before scrubbing in via a digital link.
The End of the Medical Desert
We often speak about the "digital divide" in terms of high-speed internet or the latest smartphones. But the true divide is biological. There are "medical deserts" across the globe—and even within the UK—where access to highly specialized robotic surgery is a fantasy.
Imagine a child in a remote Scottish highland or an elderly man in a rural village who requires a niche neurological repair. Currently, they are tethered to the limitations of their local hospital’s staffing.
This successful 1,500-mile link suggests a future where "centers of excellence" are no longer buildings, but networks. A world-class surgeon could perform five operations in five different cities in a single day without ever leaving their home base. This isn't about convenience for the doctor. It is about the democratization of elite skill.
However, we must be honest about the lingering shadows. The complexity of maintaining a "five-nines" (99.999%) uptime on an international data connection is immense. If the fiber-optic cable is severed by a rogue anchor in the English Channel mid-incision, what happens? The protocols for "hand-over" to the local team must be as precise as the surgery itself. We are trusting our lives not just to the steady hands of a doctor, but to the integrity of the global internet infrastructure.
The Weight of the Invisible
There is a psychological hurdle here that we haven't quite cleared. We are used to the "laying on of hands." There is a deep-seated human comfort in knowing your surgeon is in the room, that they can see the rise and fall of your chest with their own eyes, and that they share the same air you breathe.
Remote surgery asks us to place our trust in the invisible. It asks us to believe that a stream of binary code can carry the weight of a Hippocratic Oath.
But as the patient in London recovers, the data speaks louder than our ancestral fears. The surgery was a success. The margins are clear. The recovery time for robotic procedures is significantly lower than open surgery, meaning this patient will be home, sitting in their own chair, eating their own food, far sooner than they would have been twenty years ago.
The invisible stakes of this trial weren't just about one kidney. They were about the feasibility of a global surgical grid.
Beyond the Horizon
If we can bridge 1,500 miles, we can bridge 5,000. If we can bridge 5,000, we can bridge the gap between the International Space Station and Earth. We are looking at the foundational steps of extra-planetary medicine.
But back on the ground, the impact is more visceral. It is the end of the "zip code lottery" for cancer survival. It is the realization that the most precious resource in medicine—expertise—is finally being unchained from the physical world.
The surgeon in Bordeaux closes his console. He stretches his fingers, the same fingers that, moments ago, were virtually deep inside a human body in London. He walks out into the French air. 1,500 miles away, a heart beats steadily in a recovery room, a little lighter now that the weight of the cancer has been lifted by a man who was never there.
Would you like me to explore the specific cybersecurity protocols used to protect these remote surgical links from potential interference?